Cholesterol And Erectile Dysfunction
Erectile dysfunction is when a man canât achieve or maintain an erection during sex. Over the long term, high cholesterol seems to trigger a narrowing of the smaller blood vessels of the penis when they should be stretching to allow more blood for an erection . In addition, when you have too much LDL cholesterol, it can build up in arteries and then join with other substances to form plaque that hardens and narrows further blood vessels . The result can be less blood flow to both the heart and the penis, which can lead to erectile dysfunction.
Medical Conditions In Adults
- This list is presented in alphabetical order and not in order of risk.
- CDC completed an evidence review process for each medical condition on this list to ensure they met criteria for inclusion on this webpage.
- We are learning more about COVID-19 every day, and this list may be updated as the science evolves.
Lack Of Regular Exercise
If you’re inactive, fatty deposits can build up in your arteries.
If the arteries that supply blood to your heart become blocked, it can lead to a heart attack. If the arteries that supply blood to your brain are affected it can cause a stroke.
Read about the physical activity guidelines for adults aged 19 to 64.
You May Like: What Is The Relationship Between Triglycerides Cholesterol And Lipids
The Association Between Cholesterol And Heart Disease
The 20152020 Dietary Guidelines for Americans doesnt include a specific limit, it still strongly recommends eating as little dietary cholesterol as possible. It mentions studies and trials that have produced strong evidence that healthy eating patterns that are low in dietary cholesterol can reduce the risk of heart disease in adults.
An eight-week study published in 2016 stated that elevated LDL is an established risk factor for heart disease and that dietary fatty acids play a significant role in the development of heart disease. The researchers found that making minor dietary changes reduced cholesterol and could potentially reduce future risk of heart disease.
How To Prevent Coronary Heart Disease

Studies show that heart-healthy livingnever smoking, eating healthy, and being physically activethroughout life can prevent coronary heart disease and its complications.
Work with your doctor to set up a plan that works for you based on your lifestyle, your home and neighborhood environments, and your culture. Working with a team of healthcare providers may help with making changes in your diet, being physically active, managing other medical conditions, and helping you quit smoking.
Also Check: How Do You Test Cholesterol
Women And Heart Disease
Coronary heart disease is the leading cause of death for women. About 80% of women ages 40 to 60 have one or more risk factors for coronary heart disease. Having multiple risk factors significantly increases a womans chance of developing coronary heart disease.
Learn more about how the causes, risk factors, symptoms, diagnosis, and treatment of coronary heart disease may be different for women than for men. Read Advancing Women’s Heart Health to learn more.
How Is Angina Different From A Heart Attack
Both angina and heart attack are a consequence of coronary artery disease. The symptoms of a heart attack are similar to angina. But, angina is a warning symptom of heart disease, not a heart attack.
| Angina | Heart Attack |
|---|---|
| Caused by a drop in blood supply to the heart due to the gradual build-up of blockage in the arteries. | Caused by a sudden lack of blood supply to the heart muscle. The blockage is often due to a clot in a coronary artery. |
| Does not cause permanent damage to the heart. | Can cause permanent damage to the heart muscle. |
| Symptoms last a few minutes and usually stop if you rest or take medication. You may have chest pain or discomfort, shortness of breath, palpitations, fast heartbeat, dizziness, nausea, extreme weakness and sweating. Symptoms are often triggered by strenuous activity, stress, eating or being in the cold. | Symptoms usually last more than a few minutes and do not completely go away after taking nitroglycerin. Symptoms include chest pain or discomfort pain or discomfort in other areas of the upper body trouble breathing or shortness of breath sweating or cold sweat feeling full, like you are choking or indigestion nausea or vomiting lightheadedness extreme weakness anxiety fast or irregular heartbeat. |
| Emergency medical attention is not needed. Call your doctor if you have not had symptoms before or if your symptoms have gotten worse or happen more often. | Emergency medical attention is needed if symptoms last longer than 5 minutes. |
Recommended Reading: Are Potatoes Bad For Cholesterol
Living With Coronary Heart Disease
Finding coronary heart disease early can prevent it from getting worse. If left untreated, you could have a heart attack or get arrhythmias . CHD can lead to death. Proper diagnosis and treatment allows you to correct it with lifestyle changes and manage it with medicine or surgery. Surgery has various recovery timeframes.
Talk to your doctor about your specific outcomes and goals. You likely will need ongoing doctor visits and tests. CHD does increase your risk for a heart attack. Make sure you know the warning signs and when to call 911.
How Is Heart Disease Diagnosed
The diagnosis of cardiovascular disease begins by taking the patient’s history. The health-care professional needs to understand the patient’s symptoms and this may be difficult. Often, health-care professionals ask about chest pain, but the patient may deny having pain because they perceive their symptoms as pressure or heaviness. Words also may have different meanings for different people. The patient may describe their discomfort as sharp, meaning intense, while the health-care professional may understand that term to mean stabbing. For that reason, it is important for the patient to be allowed to take the time to describe the symptoms in their own words and have the health-care professional try to clarify the terms being used.
The health-care professional may ask questions about the quality and quantity of pain, where it is located, and where it might travel or radiate. It is important to know about the associated symptoms including shortness of breath, sweating, nausea, vomiting, and indigestion, as well as malaise or fatigue.
The circumstances surrounding the symptoms are also important.
- Are the symptoms brought on by activity?
- Do they get better with rest?
- Since symptoms began, does less activity provoke onset of the symptoms?
- Do the symptoms wake the patient?
These are questions that may help decide wither the angina is stable, progressing, or becoming unstable.
Read Also: How Much Cholesterol In Pork Chops
What Causes Coronary Artery Disease
CAD is caused by plaque buildup in the walls of the arteries that supply blood to the heart and other parts of the body.
Plaque is made up of deposits of cholesterol and other substances in the artery. Plaque buildup causes the inside of the arteries to narrow over time, which can partially or totally block the blood flow. This process is called atherosclerosis.
Do I Need Treatment For High Cholesterol
including whether you are also diagnosed with cardiovascular disease.Ã Many health care providers recommend treating anyone with CVD with high-dose statin therapy. This includes those with coronary heart disease and who have had a stroke.
For those who do not have CVD, treatment is determined by your individual risk for developing heart disease. Ã That risk can be estimated using calculators which factor your age, sex, medical history, and other characteristics.Ã If your risk is high , your doctor may start you on treatment preventively. They generally keep in mind your preferences towards taking medication in general.Ã For those people whose risk is unclear, a coronary artery calcium score, which is a screening test looking for calcium in the arteries, can help determine the need for statins.
For both those who have CVD and those who do not, when the decision is made to start medication, the first choice is usually a statin.
Other special groups who may need treatment:
- People with high triglyceride levels may benefit if they have other risk factors
- People with diabetes: are at high risk, and a ldl under 100 is recommended for most
- Older adults: a healthy, active older adult may benefit from the reduction you need, and be prescribed a medication accordingly.
You May Like: Are Egg Beaters Low In Cholesterol
What Can Happen If Your Arteries Become Clogged Up
If your arteries become clogged up with blood fats, your blood can’t flow around your body easily. This can lead to a number of diseases of the heart and blood vessels.
These diseases are known together as cardiovascular disease cardio refers to the heart, and vascular refers to the blood vessels.
-
Coronary heart disease
This is where the arteries have become clogged up and stiff with atherosclerosis. The blood cant flow around the body and back to the heart easily, and blood clots can form. This can lead to chest pain, heart failure, heart attacks and strokes.
-
Angina
This is a dull, heavy or tight pain in the chest which can spread to the left arm, neck, jaw or back. It happens when the arteries leading to the heart have become narrowed and the heart doesnt get enough oxygen. The pain can be brought on by exercise or activity, as the heart needs more oxygen during physical activity.
-
A heart attack
This is a medical emergency. It happens when an artery leading to the heart becomes completely blocked, often by a blood clot, cutting off the blood supply. Part of the heart muscle quickly dies, but if its treated very early the blockage can be removed.If you think you or someone you are with is having a heart attack, call 999 straight away. The signs of a heart attack include:
- a crushing pain in the chest
- sweating
- feeling weak or faint
Find out about coronavirus if you have heart disease
Signs Symptoms And Complications
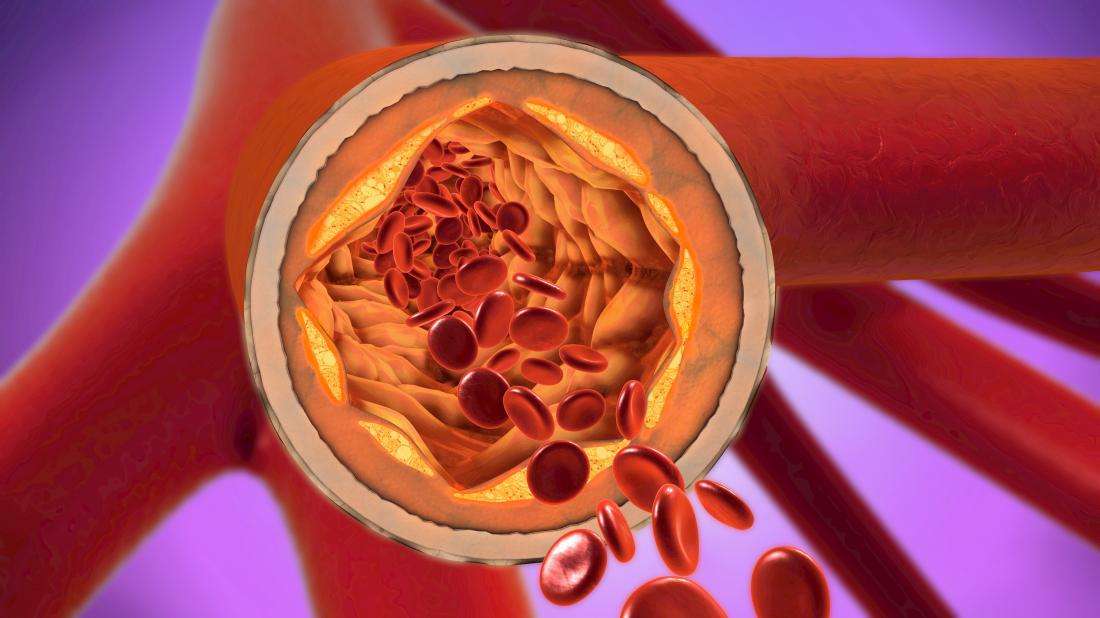
Atherosclerosis usually doesn’t cause signs and symptoms until it severely narrows or totally blocks an artery. Many people don’t know they have the disease until they have a medical emergency, such as a heart attack or stroke.
Some people may have signs and symptoms of the disease. Signs and symptoms will depend on which arteries are affected.
You May Like: Shrimp Bad Cholesterol
The Single Best Predictor Of A Heart Attack
The calcium score is the single best predictor of a heart attack. Learn about the test, plus eight other risk factors for heart disease you can’t ignore.
Each year close to 1.4 million Americans experience a heart attack, and more than 500,000 die from it. Strikingly, according to the Society for Heart Attack Prevention and Eradication, 50 to 70 percent of those who suffered fatal heart attacks were not even aware of their risk. Despite recent scientific advances in heart disease prevention, many high-risk patients are overlooked when conventional risk assessment methods such as cholesterol and blood pressure screenings are used alone.
Heres what you need to know about the No. 1 predictor of a heart attack, the calcium score, plus eight other risk factors to consider.
Where Are The Coronary Arteries What Do They Do
Coronary arteries are the blood vessels that supply oxygen-rich blood to your heart muscle to keep it pumping. The coronary arteries are directly on top of your heart muscle. You have four main coronary arteries:
- The right coronary artery.
- The left anterior descending artery.
- The left circumflex artery.
Don’t Miss: Is Shrimp Bad For Your Cholesterol
What About Medications
Statins are the most well-researched medications for lowering cholesterol. They can lower your risk for heart disease if youre already at high risk.
However, there are a few important things to note about statins and cholesterol medications:
-
While many medications can lower cholesterol levels, only some, such as statins, have been shown to reduce the risk of heart disease.
-
Whether or not you would benefit from a cholesterol medication depends on your overall risk for heart disease. Healthcare providers estimate this risk based on your cholesterol levels as well as other factors mentioned above .
-
If youve already had a heart attack or stroke, you are at high risk for a second heart attack or stroke. Many people with this risk should be on statins. But talk to your healthcare provider about whether a statin is right for you.
Some other cholesterol-lowering medications that your provider may recommend in addition to statins are listed below.
Your provider may also recommend other medications to help with high cholesterol, such as the following:
-
Fibrates, niacin, and omega-3 fatty acids lower triglyceride levels.
-
Bile acid sequestrants cause your body to get rid of bile acids. Your liver then uses up cholesterol from your bloodstream to replace the lost acids.
What Is A Heart Attack
A heart attack occurs when oxygenated blood cannot get to a section of your heart. That section becomes damaged from lack of oxygen and begins to die. Heart attacks usually stem from coronary artery disease.
Sometimes heart attacks occur without any warning, called silent heart attacks although most people experience some sort of symptom before the actual attack. The most common symptoms are chest pain or pain in the upper body, arms, back, neck, jaw, or stomach. Occasionally, patients have difficulty breathing, experience nausea or vomiting, or break out in a cold sweat. As with CAD, women are more likely to have atypical symptoms, especially if very young or very old. The important thing to remember is that symptoms vary, so if you feel like something is not right, listen to your body and get help.
If we suspect that you have had a heart attack, we start by providing oxygen and medications such as aspirin and nitroglycerin . We work to restore blood flow to your heart. If the attack was caused by a blood clot in your heart, we may use medication to dissolve the blood clots or perform an angioplasty, an emergency procedure that opens up the blockage in the artery or to stop additional clotting, reduce the strain on the heart, and prevent further attacks.
Recommended Reading: How Much Cholesterol In Egg Beaters
What Are The Signs And Symptoms Of Heart Disease
- The classic symptoms of angina, or pain from the heart, are described as a crushing pain or heaviness in the center of the chest with radiation of the pain to the arm or jaw. There can be associated shortness of breath sweating and nausea.
- The symptoms tend to be brought on by activity and get better with rest.
- Some people may have indigestion and nausea while others may have upper abdominal, shoulder, or back pain.
- Unstable angina is the term used to describe symptoms that occur at rest, waken the patient from sleep, and do not respond quickly to nitroglycerin or rest.
Other heart disease symptoms and signs
Not all pain from heart disease have the same signs and symptoms. The more we learn about heart disease, the more we realize that symptoms can be markedly different in different groups of people. Women, people who have diabetes, and the elderly may have different pain perceptions and may complain of overwhelming fatigue and weakness or a change in their ability to perform routine daily activities like walking, climbing steps, or doing household chores. Some patients may have no discomfort at all.
Often the first signs and symptoms of heart disease may be a heart attack. This can lead to crushing chest pressure, shortness of breath, sweating, and perhaps sudden cardiac death.
What Are Ldl And Hdl
LDL and HDL are two types of lipoproteins. They are a combination of fat and protein. The lipids need to be attached to the proteins so they can move through the blood. LDL and HDL have different purposes:
- LDL stands for low-density lipoproteins. It is sometimes called the “bad” cholesterol because a high LDL level leads to a buildup of cholesterol in your arteries.
- HDL stands for high-density lipoproteins. It is sometimes called the “good” cholesterol because it carries cholesterol from other parts of your body back to your liver. Your liver then removes the cholesterol from your body.
Read Also: Pork Chops Cholesterol
Treatment For Coronary Heart Disease
Treatment may include:
-
Modification of risk factors. Risk factors that you can change include smoking, high cholesterol levels, high blood glucose levels, lack of exercise, poor dietary habits, being overweight, and high blood pressure.
-
Medicines. Medicine that may be used to treat coronary artery disease include:
-
Antiplatelets. These decrease blood clotting. Aspirin, clopidogrel, ticlopidine, and prasugrel are examples of antiplatelets.
-
Antihyperlipidemics. These lower lipids in the blood, particularly low density lipid cholesterol. Statins are a group of cholesterol-lowering medicines, and include simvastatin, atorvastatin, and pravastatin, among others. Bile acid sequestrants–colesevelam, cholestyramine and colestipol–and nicotinic acid are other medicines used to reduce cholesterol levels.
-
Antihypertensives. These lower blood pressure. Several different groups of medicines work in different ways to lower blood pressure.
Coronary angioplasty. With this procedure, a balloon is used to create a bigger opening in the vessel to increase blood flow. Although angioplasty is done in other blood vessels elsewhere in the body, percutaneous coronary intervention refers to angioplasty in the coronary arteries to permit more blood flow into the heart. PCI is also called percutaneous transluminal coronary angioplasty . There are several types of PCI procedures, including:
Balloon angioplasty. A small balloon is inflated inside the blocked artery to open the blocked area.
Cardiovascular Diseases Risk Assessment

Absolute prediction of CVD risk of a person can be made using prediction charts issued or published by the WHO and ACC/AHA. The recommendations are made for management of major cardiovascular risk factors through changes in lifestyle and prophylactic drug therapies.
The ACC/AHA have produced guidelines for the procedures of detection, management, or prevention of CVD. In November 2013, The ACC and AHA released updated risk-assessment guidelines for atherosclerotic CVD. Changes and recommendations include the following.
Guidelines from AHA/ACC recommend use of a revised calculator for estimating the 10-year risk of developing a first ASCVD event, which is defined as a nonfatal MI, death from CHD, or stroke in a person who was initially free from ASCVD. The calculator incorporates the following risk factors: sex, age, race, total cholesterol, HDL, systolic blood pressure, treatment for elevated blood pressure, diabetes, and smoking.
For patients 2079 years of age who do not have existing clinical ASCVD, the guidelines recommend assessing clinical risk factors every 46 years. For patients with low 10-year risk , the guidelines recommend assessing 30-year or lifetime risk in patients 2059-year-old.
Don’t Miss: Potatoes And Triglycerides